Everything about Cartilage Restoration Surgery
Living with persistent knee pain doesn’t just affect your joint; it gradually changes how you live your life. You might hesitate on stairs or avoid activities you once enjoyed, and over time, that can impact both mobility and confidence.
At the centre of this issue is the cartilage in the knee, a smooth layer that helps your knee move easily. As it wears down, stiffness, discomfort, and reduced movement often follow.
While older approaches focused on simply “cleaning up” the joint, modern orthopedics has moved far beyond that. Today, the focus has shifted away from temporary fixes towards knee cartilage restoration and regeneration, which aim to repair or rebuild the joint surface.
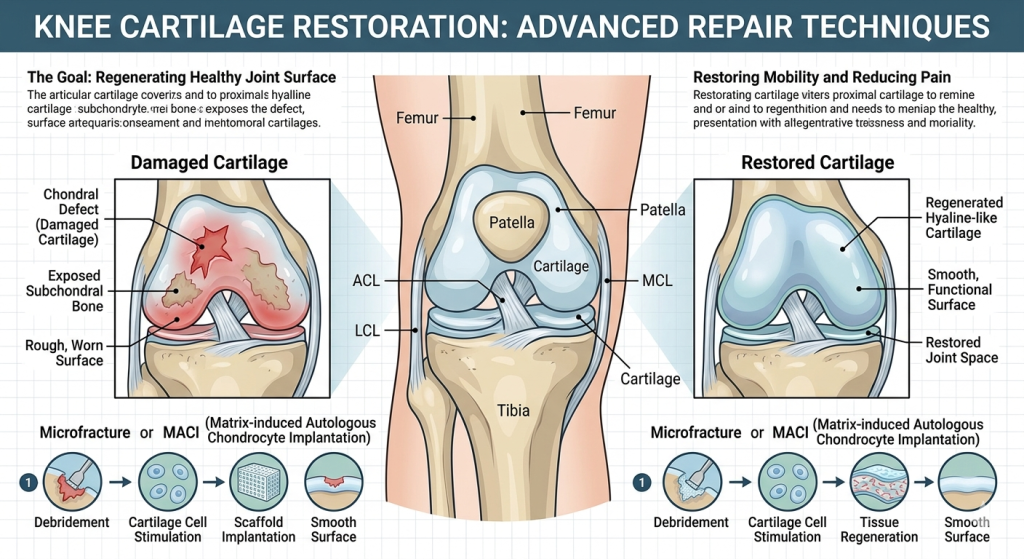
This naturally raises an important question: what is knee cartilage restoration surgery? Rather than just managing symptoms, it involves restoring damaged cartilage to improve both function and long-term joint health.
With a strong emphasis on preserving natural joint function, Dr. Rik Kundra, a specialist knee surgeon in Dubai, approaches treatment with a long-term view: supporting sustained mobility rather than short-term fixes.
What is Cartilage in the Knee and why can't it heal itself?
Cartilage in the knee is a specialized, smooth tissue that covers the ends of your bones where they meet to form the joint. It acts as a natural shock absorber, allowing your knee to move freely and painlessly during everyday activities like walking, bending, and running.
Unlike muscles or skin, cartilage has no direct blood supply. This is the key reason why it struggles to repair itself.
Here’s what that means in practical terms:
- No blood flow = limited healing cells reaching the damaged area
- No nutrients delivered directly to support repair
- No strong inflammatory response, which is usually needed for healing
As a result, once cartilage is damaged, whether due to injury, wear and tear, or aging, it tends to degenerate further over time rather than regenerate.
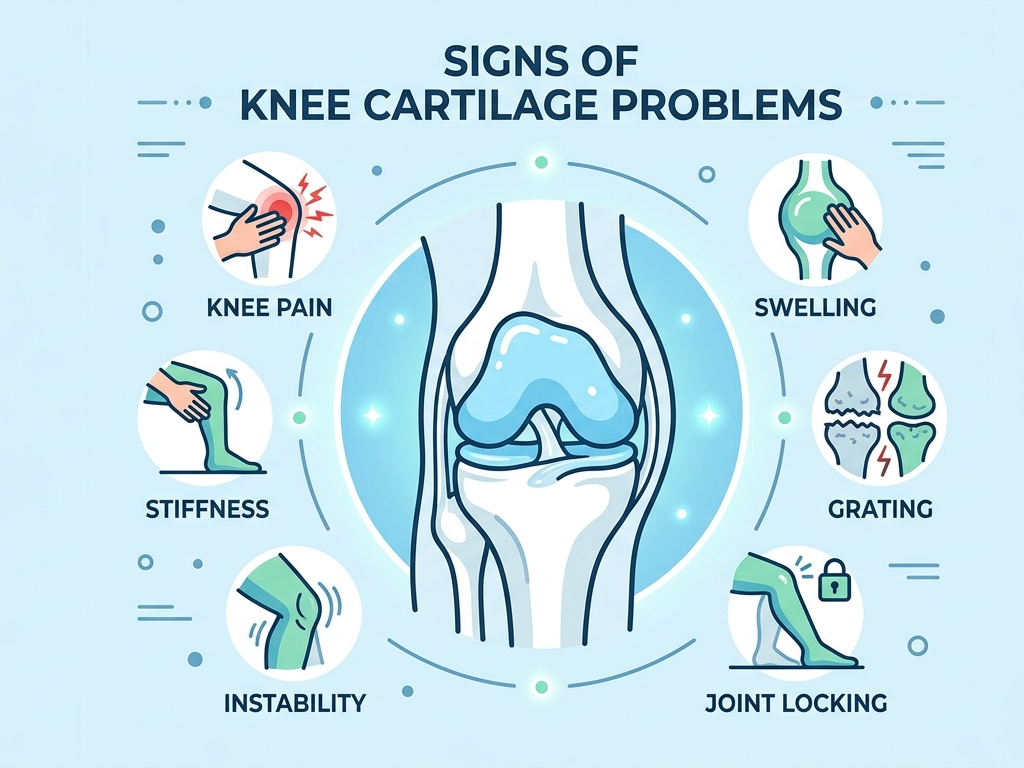
Signs you may have a Knee Cartilage problem
Knee cartilage damage doesn’t always happen suddenly. More often, it develops gradually, starting with mild discomfort and becoming more noticeable over time:
- Ongoing pain that doesn’t settle with rest
- Catching, clicking, locking, or a sense of the knee “giving way”
- Swelling, especially after activity or long periods on your feet
- Difficulty bending or straightening your knee
- Swelling, especially after activity or long periods on your feet
Important: These symptoms overlap with many other knee conditions. An accurate diagnosis is essential before any treatment decision is made. Self-diagnosis based solely on symptoms can delay appropriate care. |
How is Knee Cartilage damage diagnosed?
A thorough diagnostic workup includes clinical assessment, imaging, and sometimes arthroscopic evaluation.
MRI scanning is the gold standard for assessing cartilage damage, clearly showing the location, size, and depth of defects, as well as surrounding structures such as bone, ligaments, and meniscus.
In some cases, diagnostic arthroscopy (keyhole camera inspection of the joint) is used to directly assess cartilage quality, offering insights that imaging alone may not fully capture, especially when planning cartilage repair or knee cartilage surgery.
What is Knee Cartilage Restoration surgery?
Knee cartilage restoration surgery refers to a group of advanced procedures designed to restore damaged cartilage in the knee joint, helping reduce pain, improve movement, and protect the joint over the long term.
Importantly, it doesn’t usually mean replacing the whole knee. The focus is on treating the damaged area while preserving as much of your natural joint as possible.
Rather than simply removing worn-out tissue, modern approaches focus on knee cartilage restoration and repair, rebuilding the joint surface to support smoother movement and better long-term function.
This makes it a more joint-preserving alternative to traditional solutions, especially for active patients or those looking to delay full knee replacement.
Also Read – Everything About Knee Cartilage Damage
Knee Cartilage Regeneration & Restoration: Your full range of options
One of the most common misconceptions is that knee cartilage restoration surgery is a single procedure. In fact, it includes various techniques, each with different needs, mechanisms, and outcomes.
Simple Microfracture
Ideal for small cartilage defects, this minimally invasive procedure uses a small tool to make tiny holes in the bone beneath the damaged cartilage.
The holes allow bone marrow cells to enter the area, forming a clot that develops into new cartilage-like tissue. While simple and effective, the new fibrocartilage is not as strong as your original cartilage.
OATS surgery (Osteochondral Autograft Transfer)
OATS surgery treats small areas of cartilage damage by taking healthy cartilage from another part of the knee and transplanting it to the injured spot.
This knee cartilage transplant restores a smooth joint surface and is especially useful for active patients who want to maintain mobility and function.
Knee Chondroplasty
A knee chondroplasty smooths rough or loose cartilage and removes any abnormal tissue or excess bone.
By cleaning and reshaping the joint surface, it reduces pain, improves mobility, and allows healthy cartilage to grow over time.
Osteochondral Allograft
Used for larger or deeper cartilage defects, this procedure involves taking cartilage tissue from a donor, sterilising it, and transplanting it to the injured area.
An allograft provides a strong, natural cartilage surface when an autograft (your own cartilage) isn’t enough.
Synthetic / gel-based options
Emerging treatments like knee cartilage restoration gel or other biomaterials can support cartilage healing and improve joint function.
These cartilage restoration knee solutions are especially useful for patients who may not be candidates for traditional grafts.
Knee Realignment surgery (Osteotomy)
Osteotomy is used when knee alignment is causing extra pressure on damaged cartilage.
The bone is carefully cut and repositioned to shift weight away from the affected area, protecting repaired cartilage and improving long-term outcomes.
Knee Replacement surgery
For severe or widespread cartilage loss, partial or total knee replacement (knee arthroplasty) replaces the damaged joint with a prosthetic implant.
This relieves pain, restores function, and is considered when joint-preserving options are no longer sufficient.
Knee Cartilage Transplant success rateAbout 75-90% of patients experience significant pain relief and improved knee movement, especially with early intervention and proper rehab. |
What to expect: The patient journey
Deciding to undergo knee cartilage restoration surgery is never a small step. It’s a shift from managing a problem to actively improving your health.
The journey with Dr. Rik is designed to be clear and supportive, ensuring you feel like a partner in your own recovery rather than just a patient on a schedule.
The decision: When are you ready?
There is no “perfect” time for surgery, but there is a right time for you.
You are likely ready for cartilage restoration surgery when the “conservative” options, like physical therapy or injections, no longer allow you to live the life you want.
If you are avoiding activities you love or planning your day around your knee pain, it’s time to move toward a more permanent form of knee cartilage repair.
Recovery & rehabilitation
Recovery is a gradual process, focused on evidence-led progress rather than instant results.
- The early phase: The first few weeks focus on protecting the new cartilage. You may use crutches or a brace to limit weight-bearing while the “biological graft” takes hold.
- The strengthening phase: Once the tissue is stable, you’ll work through a guided physiotherapy program. This isn’t about rushing; it’s about rebuilding the muscles that support your new joint surface.
- The return to action: Most patients see significant improvement in daily comfort within a few months, but full maturation of the cartilage can take up to a year.
Knee Cartilage Restoration surgery cost
Understanding the financial aspect is part of feeling secure in your care.
While knee cartilage restoration surgery cost varies depending on the specific technique used, such as a knee cartilage transplant or cell-based knee cartilage regeneration, it is helpful to view it as a long-term investment in your mobility.
Choosing an experienced specialist and the right approach can significantly reduce the “hidden costs” of healthcare, like the need for revision surgeries, prolonged time off work, or future joint replacements.
Why does choosing the right knee surgeon matter?
Getting the right outcome in Knee Cartilage Restoration isn’t just about the procedure itself. A skilled surgeon not only performs the procedure accurately but also create a treatment plan tailored to your knee, your lifestyle, and your long-term joint health for effective Knee Cartilage Regeneration.
Dr. Rik Kundra: Knee preservation & restoration specialist
With 19+ years of experience in orthopedic surgery and sports medicine, Dr. Rik Kundra is a leading expert in knee joint preservation, biologic reconstruction, and cartilage repair. He is highly respected for treating athletes, active adults, and younger patients with knee arthritis or cartilage injuries.
His approach is evidence-based and patient-focused, with an emphasis on preserving the natural knee wherever possible, rather than moving straight to replacement.
Ready to discuss your options?
Scheduling a consultation can help you determine the best approach to restore mobility, reduce pain, and protect your natural knee for the long term.
FAQ's On Knee Cartilage Restoration
Because cartilage in the knee acts as a shock absorber, damage increases friction, causing swelling, catching, and deep aching pain. Over time, this can affect how comfortably your knee moves.
Unfortunately, no. Cartilage has no blood supply or nerves, so it cannot heal itself. Diet and supplements may support joint health, but they won’t replace lost cartilage. Knee cartilage restoration surgery is required to “trigger” the healing process.
The ideal candidate is someone with a focal (localized) injury, a stable knee (healthy ligaments), and a desire to remain active. It is generally not recommended for those with advanced, widespread osteoarthritis.
While true knee cartilage regeneration cannot occur naturally, certain lifestyle measures can support joint health and slow further damage. These include maintaining a healthy weight, engaging in low-impact exercise, strengthening surrounding muscles, and following a balanced diet. However, these approaches do not replace lost cartilage.
This depends on the size, location, and depth of your cartilage loss. During your consultation, Dr. Rik Kundra uses advanced imaging (MRI) and a physical exam to determine if knee cartilage restoration, a knee cartilage transplant, knee cartilage gel, or knee cartilage regeneration is the best fit for your lifestyle.
Some discomfort is normal post-surgery, but modern techniques and pain management strategies ensure gradual improvement, with most patients returning to daily activities within weeks.
Disclaimer
All content and media on this page are created and published for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Meet Dr. Rik personally for appropriate medical diagnosis and advice.
Medically reviewed by Dr rik kundra


